Understanding Mucus in Chronic Obstructive Pulmonary Disease (COPD)
Mucus plays a major role in Chronic Obstructive Pulmonary Disease (COPD), especially in the Chronic Bronchitis phenotypes. Mucus increases airway resistance making it harder for the patient to breath. At the same time mucus impedes regional ventilation thereby disturbing the ventilation/perfusion matching and perturbing deposition patterns of inhalation medication. Mucus production and transport however is notoriously heterogeneous making it very hard to study with conventional lung function tests such as spirometry (eg FEV1). Functional Respiratory Imaging (FRI) provides a direct measure of regional ventilation and airway resistance which enables better understanding of the heterogeneity of the disease and, when applied in clinical trials, the heterogeneity of the treatment effect.
Direct measurements of the anatomical structures, increasingly in combination with A.I., offers new opportunities to enhances respiratory drug development and care.
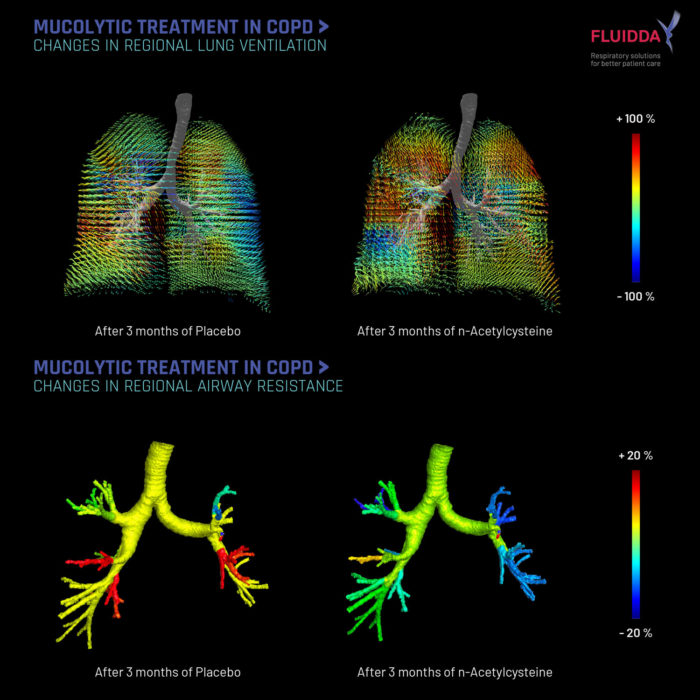
In the figure above the effect of n-Acetylcysteine (nAC) and placebo on regional ventilation and airway resistance is demonstrated in a COPD patient with low Glutathione peroxidase (GPx). One can observe that nAC reduces airway resistance and enhances regional ventilation [1]. At the same time the heterogeneity of the disease and treatment is also apparent from this case.
Be sure to follow us on on LinkedIn to make sure you don’t miss out on any FRI-related research!
Categorised in: Research / October 24, 2019 4:31 pm /
Tags: COPD, Mapping, Mucus, Ventilation